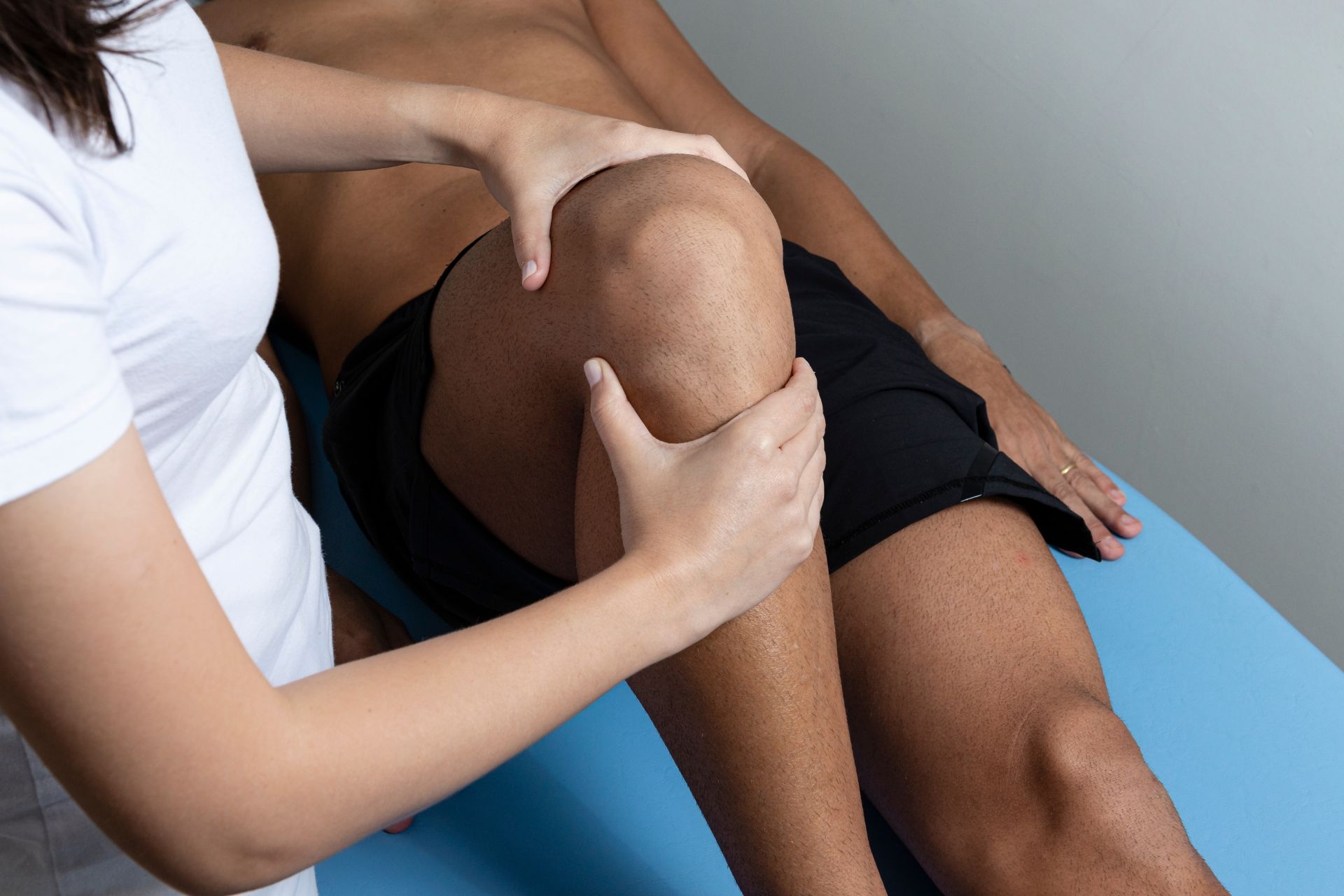
Tendon Palpation
How can the presence of crepitus during tendon palpation indicate a potential injury or degenerative condition?
The presence of crepitus during tendon palpation can indicate a potential injury or degenerative condition by suggesting the presence of irregularities or roughness in the tendon structure. Crepitus is characterized by a crackling or popping sensation felt when the tendon is palpated, which may be caused by friction between roughened surfaces or the presence of loose fragments within the tendon. This abnormal texture can be a sign of tendon damage, inflammation, or degeneration, prompting further investigation into the underlying condition.