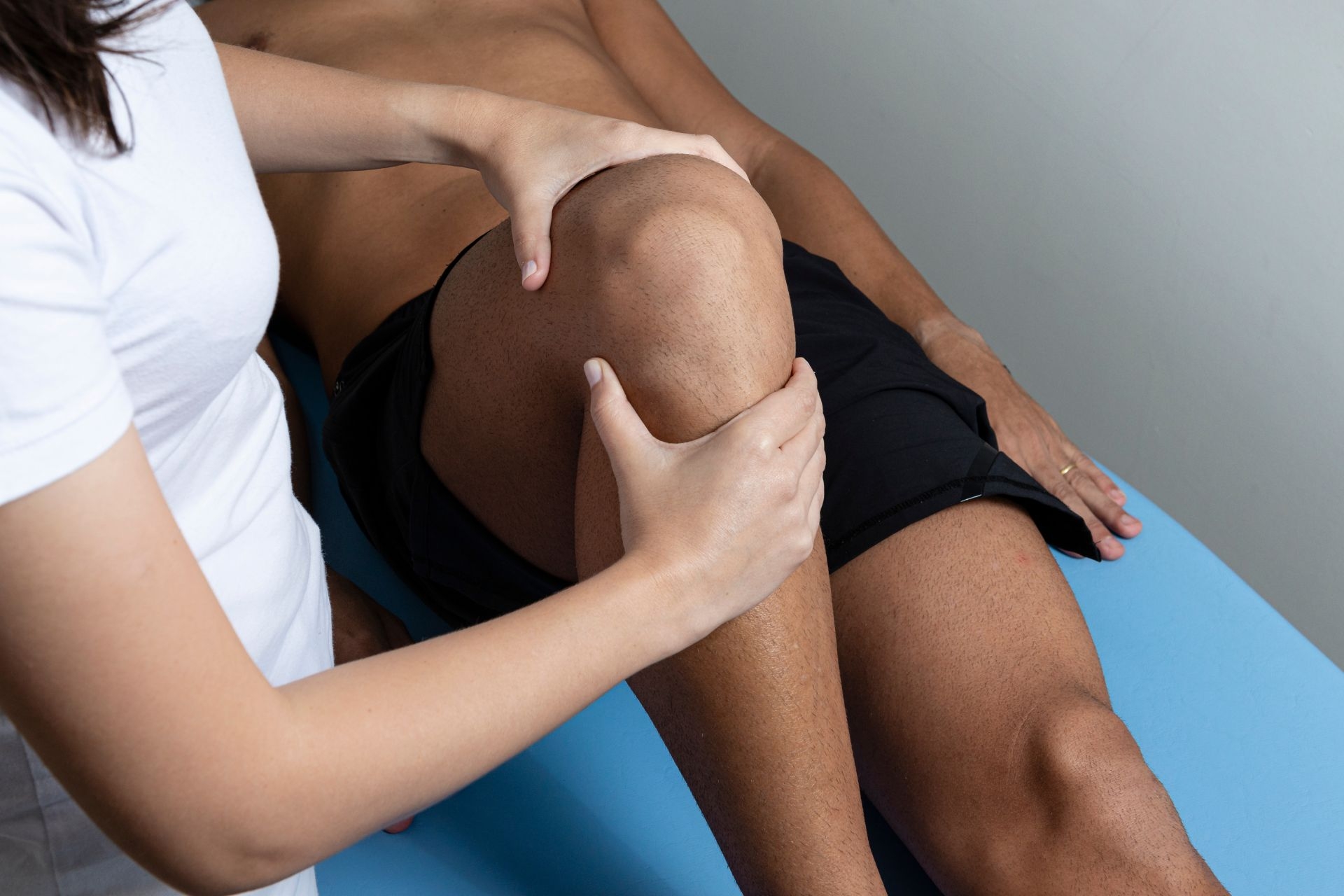
Neural Tension Testing
How is neural tension testing used to assess nerve mobility and function?
Neural tension testing is utilized to evaluate the mobility and function of nerves in the body. This test involves applying controlled tension to specific nerves to assess their response and determine if there are any restrictions or abnormalities in nerve movement. By performing neural tension testing, healthcare providers can identify issues such as nerve entrapment, inflammation, or dysfunction that may be causing symptoms in patients.