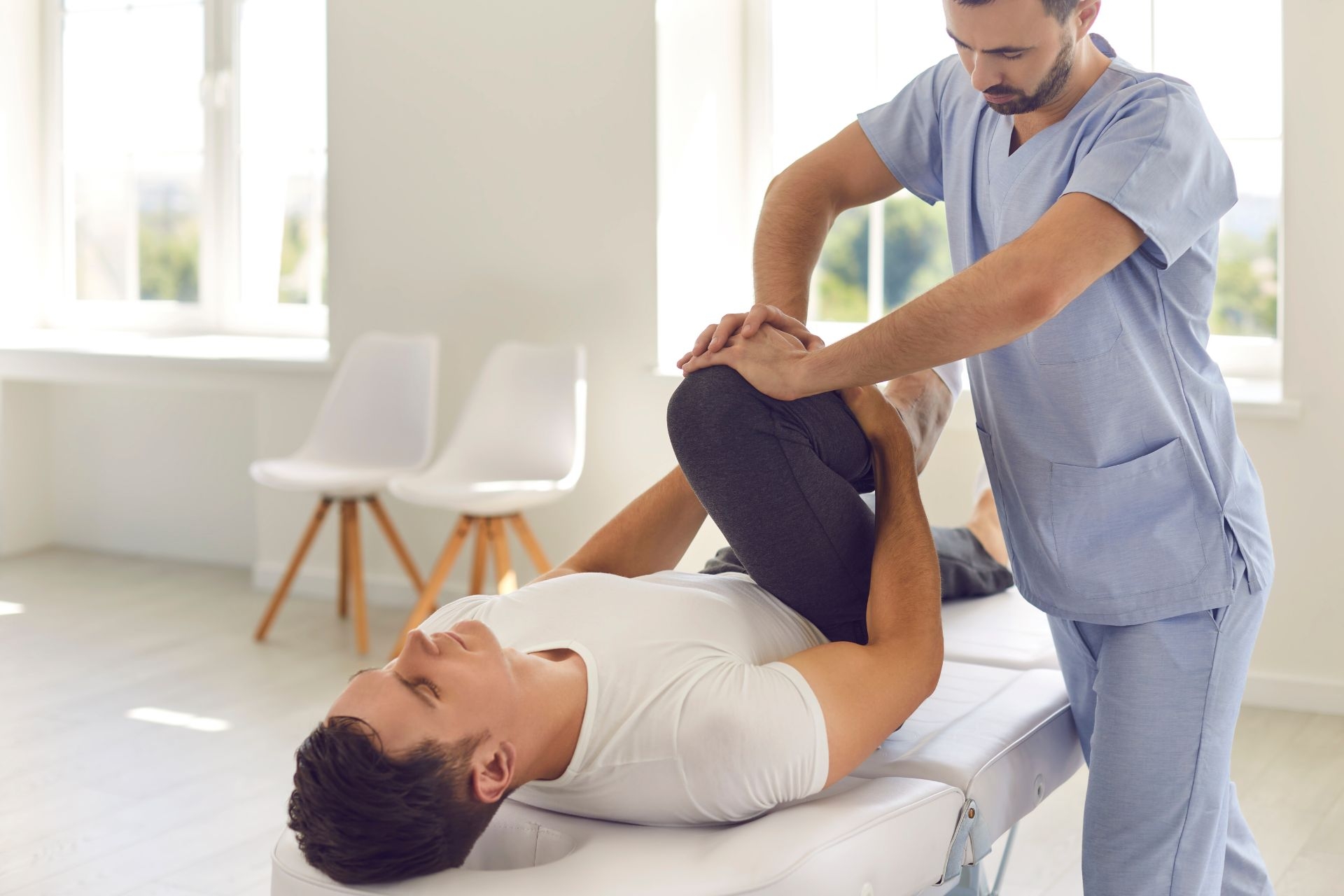
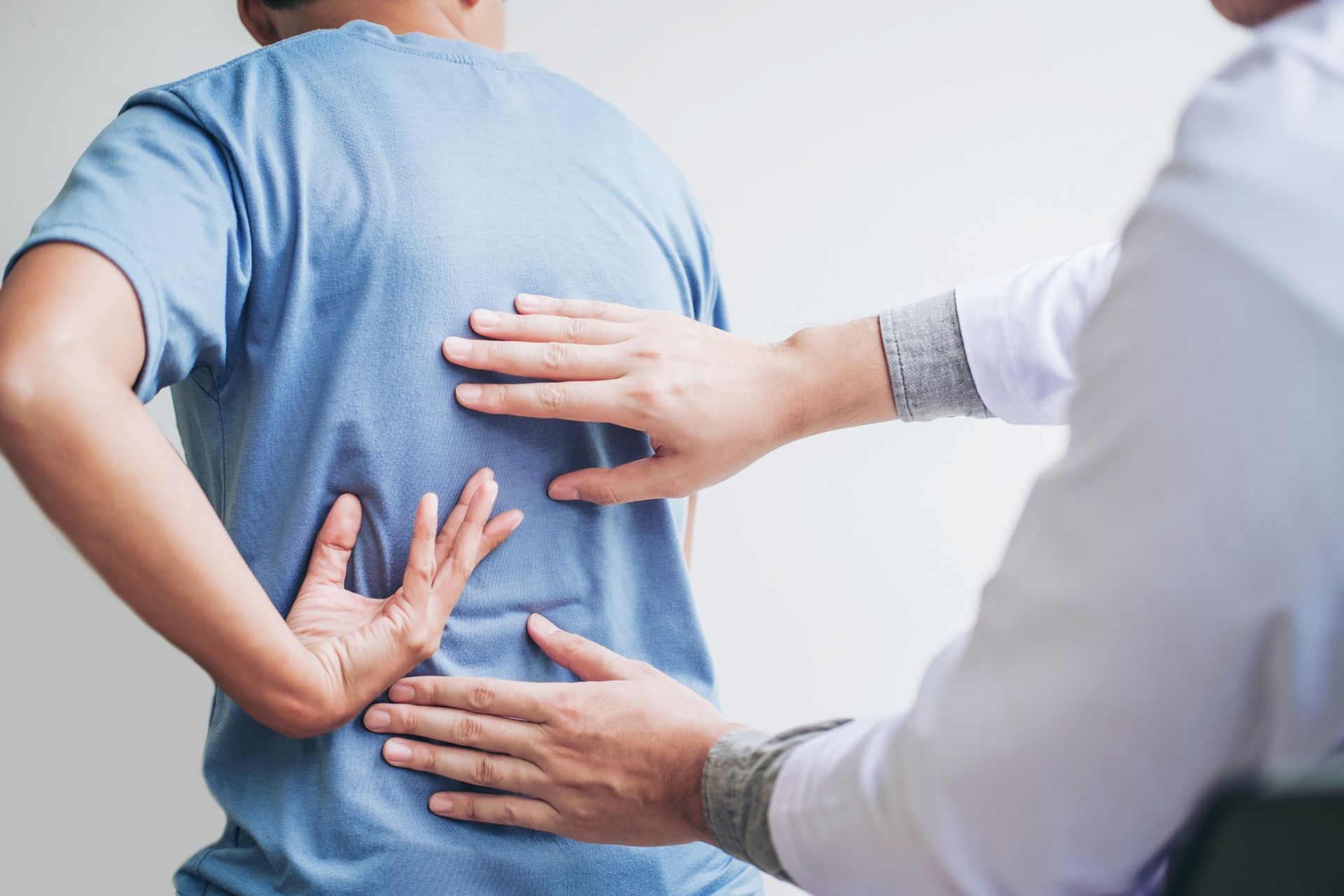
Myofascial Release
How does myofascial release help with trigger points in the muscles?
Myofascial release helps with trigger points in the muscles by applying sustained pressure to the affected areas, which helps to release the tension and tightness in the fascia surrounding the muscles. By targeting these trigger points, myofascial release can help to alleviate pain, improve circulation, and restore proper function to the muscles. This technique can help to break up adhesions and knots in the muscle tissue, allowing for better movement and reduced discomfort.